Orthopedics
Our therapists use several different types of treatments and techniques that are proven to reduce pain and inflammation to get you back on your feet.

Expert Orthopedic Care
Our team of specialized Orthopedic Therapists will guide patients through rehabilitation after injury or surgery to improve mobility, increase strength, and enhance function. They design personalized treatment plans involving manual therapy, exercises, stretches, modalities, and functional activity.
Orthopedics Programs
Back in Action
Our mission is to help you reclaim your active lifestyle and get back to doing the things you love. Whether it’s mastering higher level activities like Barre, Yoga, or Fitness Classes, lifting your grandchild with ease, or simply maintaining an active lifestyle, we’re here to support you every step of the way!
Let our Therapists get you Back in Action. They will help you:
- Understand your condition
- Achieve your fitness goals
- Strive for excellent health
- Listen and work with therapists to determine an individualized treatment plan
- Participate actively in the treatment program
- Continue an active lifestyle
Don’t let pain or discomfort hold you back from living your best life. Our therapists are dedicated to getting you back to the activities that bring you joy. Let’s work together to put you back in control of your health and wellness!

Anti-Gravity Treadmill
Anti-Gravity Treadmills utilize cutting edge technology to help get you back to enjoying life pain free. Athletes from the NFL, NBA, MLB, NHL, and many other professional organizations utilize the unique unweighting capabilities of the treadmills.

The benefits of controlling gravity and reducing body weight include:
- Reducing the impact of physical activity on joints
- Safely progressing to full weight bearing activities in a controlled environment
- Adding weight bearing activity soon after surgery
- Improve mobility, strength, and safety
- Utilizing the same rehabilitation technology as professional athletes
Aquatic Therapy
Aquatic physical therapy provides the benefit of exercise with little or no stress on joints or muscles, and swimming ability is not required. The natural buoyancy of water reduces the natural forces exerted on our bodies which makes exercises easier to perform in comparison to land-based activities. The viscosity of water provides resistance for strength training, and the hydrostatic pressure helps to support the body and improves positional awareness providing a safe workout environment.
Aquatic physical therapy is designed to improve an individual’s functioning, balance/coordination, body mechanics, flexibility, and/or muscle tone.
Our programs are developed by licensed physical therapists and are tailored to most conditions including:
- Arthritis
- Athletic Injuries
- Back & Joint Problems
- General Deconditioning
- Fibromyalgia

Blood Flow Restriction
What is BFR?
Blood flow restriction (BFR) therapy is a way to increase strength or endurance without stressing injured areas through heavy loads or prolonged movement.

How does it work?
- BFR utilizes a specialized wide tourniquet at the top of the arms or legs to limit arterial flow and slow venous return. The tourniquet pressure is determined by a special machine that assesses the minimal amount of pressure needed based on your individual blood pressure.
- The tourniquet system used for BFR training is designed to limit oxygen to the limb to generate a hypoxic event that leads to a cascade of chemical changes that are vital for muscle protein synthesis. BFR allows us to minimize muscle protein breakdown while still producing muscle protein synthesis and therefore muscle growth.
Who can Benefit from it?
BFR therapy can be used by a wide variety of populations. It is often used by athletes both amateur and professional and can be beneficial for patients who have failed to respond to traditional strengthening techniques.
Hand Therapy
At Physical Therapy at St. Luke’s, we have occupational and physical therapists who specialize in hand therapy. We treat a variety of diagnoses involving the whole upper extremity, including the shoulder, elbow, wrist, and hand. Our hand therapists are trained in providing individualized treatment plans, fabricating custom protective and dynamic orthoses, and delivering optimal care.
- Tendon or Nerve Repair
- Fractures
- Sprains and Strains
- Crush Injuries
- Joint Instability
- Arthritis/Joint Replacement
- Pain-Related Syndromes
- Carpal Tunnel Syndrome
- Cubital Tunnel Syndrome
- Radial Tunnel Syndrome
- Thoracic Outlet Syndrome
- Tennis Elbow
- Golfer’s Elbow
- De Quervain’s Tenosynovitis
- Trigger finger
- ECU tenosynovitis

Laser Therapy
Deep Tissue Laser Therapy™ is a scientifically proven way to reduce pain and inflammation. Treatments are fast, safe, painless and most patients experience results after only a few sessions.
Laser Therapy’s healing effects include:
- Improved blood circulation
- Pain relief
- Reduction of swelling and inflammation
- Enhanced mobility and flexibility of stiff joints
Common Conditions Treated Include:
- Muscle/Tendon Injuries
- Joint Pain
- Head, Neck, & Back Pain
- Carpal Tunnel Syndrome
- Post-Surgical Recovery

Manual Therapy
Manual therapy is defined as the skilled, specific passive movement of joints and soft tissues applied at varying speeds and amplitudes in order to:
- Reduce pain
- Increase range of motion
- Reduce or eliminate soft tissue inflammation
- Induce relaxation
- Improve tissue repair, extensibility and/or stability
- Facilitate movement
- Improve function
- Provide long lasting relief
Some common procedures include:
- Spinal and peripheral joint mobilization
- Manual soft tissue mobilization
- Instrument assisted soft tissue mobilization
- Trigger point therapy
- Myofascial release
- Counterstain
Our expert physical therapists can determine if manual therapy is the right fit for your individual needs and goals by performing a thorough evaluation.

Orthotics
Custom Orthotics help your feet function in their optimal neutral position and eliminate the need for your body to compensate for malalignment in your feet.
- Individualized – they match the contours of your feet and are designed to work the way that you are.
- Support for your feet – they help to provide comfort when standing for long periods of time.
- Prevent future injuries – they help normalize your gait while walking and running.
- Versatile – styles range from athletic shoes to dress shoes, including pediatric and diabetic shoes.

The Benefits of Orthotics:
- Heel pain/Plantar Fasciitis
- Arch pain/High arches
- Flat feet
- Knee pain
- Lower back pain
- Hip pain
- Leg fatigue
- Corns & calluses
- Bunions
- And more!
Redcord Suspension System
Originating from Norway in the early 1990’s, Redcord Suspension System utilizes an anti-gravity suspension system and sling-based exercises with a focus on neuromuscular activation (NEURAC). NEURAC aims to restore functional movement patterns by utilizing bungee-assisted suspension exercises to allow for isolated and controlled movements focusing on reversing the pain cycle. Goals of the Redcord Suspension System include eliminating or reducing pain, optimizing neuromuscular control, restoring normal range of motion, and/or enabling the patient to tolerate exercise and physical therapy.

Common conditions treated with Redcord Suspension System:
- Lower back pain
- Sciatica
- Shoulder impingement syndrome
- Rotator cuff tears
- Bursitis (including hip or shoulder)
- Tendinitis/Tendinopathy
- Neck pain
- Whip lash injury
- Joint replacements (including knee or hip)
- ACL reconstruction
- Heel Pain
- Balance and gait dysfunction
- Parkinson’s Disease
- Multiple Sclerosis
- Spinal cord Injury
Scoliosis
Adolescent Idiopathic Scoliosis (AIS) is the most common type of Scoliosis and is a condition that impacts the development of the spine in adolescents. It is both a structural and functional change, and physical therapists play an important role in managing it effectively!
Modern Physical Therapy Scoliosis treatment is built on practices that have been working for over 100 years, such as those introduced by Schroth, Rigo, and other methods.
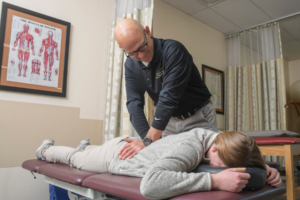
Physical Therapy for Scoliosis is…
- Individualized – We examine many elements of the patient such as their curve, posture, diagnostic imaging, strength and mobility to make treatment plans that are specific to each patient’s needs and presentation.
- Focused – Each patient is unique with different limitations and varied goals and priorities. Our therapists will promote a plan of care that works towards these goals making them the emphasis of our outcomes.
- Empowering – Scoliosis is a condition that can seem alarming and overwhelming. Our therapy approach helps to empower patients and families with the knowledge and the confidence needed to achieve success and the tools to self-manage this condition.
- Collaborative – Our therapists work side-by-side with other specialists including orthopedic surgeons and orthotists to ensure that each patient case and concerns are being addressed thoroughly and effectively.
Benefits of Physical Therapy for Scoliosis:
- Improved postural control
- Reduce pain and discomfort
- Better strength and endurance
- Reduce curve progression
While Scoliosis can be identified in children at a much earlier age, the best time to pursue physical therapy treatment is during adolescence when bone growth and maturity is happening most rapid. Changes made at this time have the best chance of being effective over the long-term.
Shockwave Therapy
What is Shockwave Therapy?
Shockwave Therapy is a highly effective, non-invasive treatment method that accelerates the healing of injured body tissues. It uses a unique set of pressure waves focused on the injury site to stimulate metabolism, enhance blood circulation, and accelerate the healing process. Damaged tissue gradually regenerates and eventually heals.

Shockwave can be used to treat acute or chronic muscle, tendon, or soft tissue pain that significantly impairs mobility or quality of life including:
- Plantar Fasciitis
- Frozen Shoulder
- Tennis Elbow
- Tendinitis/Bursitis
- Myofascial Trigger Points
The Benefits of Shockwave Therapy:
- Non-invasive
- No anesthesia
- No risk of infection
- No scarring
- No downtime
- Over 80% patient satisfaction
- Faster, easier healing process
TMJD Therapy
What is TMJD?
Temporomandibular Joint Dysfunction (TMJD) is a general term for a group of conditions that affect the temporomandibular joint — the joint on each side of your head in front of your ears, where your lower jawbone meets your skull. This joint allows you to open and close your mouth. TMJD is characterized by pain of the jaw joint that is made worse during or after eating or yawning. It can cause limited jaw movement and clicks and pops during chewing. In severe cases, pain can radiate into the neck, shoulders and back.
Signs and Symptoms of TMJD Disorders May Include:
- Pain or tenderness of your jaw
- Aching pain or pressure in and around your ear
- Pain in the neck and shoulders
- Difficulty chewing or discomfort while chewing
- Aching facial pain
- Locking of the joint, making it difficult to open or close your mouth
- Jaw muscle stiffness
- Headache
- A bite that feels “off”
Why Choose Physical Therapy for TMJD?
Scientists strongly recommend treating TMJD with the most conservative approaches possible, including physical therapy interventions. These are treatments that do not cause permanent changes in, or change the structure or position of, the jaws or teeth. Even when these disorders have become persistent, most patients still do not need aggressive types of treatment as research has shown that irreversible aggressive treatments may even make the problem worse.
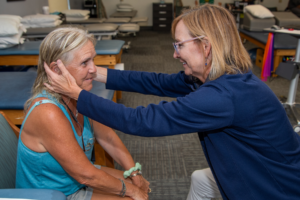
Vestibular & Fall Prevention
What is a Vestibular Disorder?
The disorder develops when the vestibular system, made up of the inner ear and brain (which help control balance and eye movements) is damaged by disease, aging, or injury.
Benefits of Vestibular Therapy:
- Decreasing the risk of falling
- Decreasing intensity and/ or episodes of vertigo/dizziness
- Improving balance and ambulation
- Improving eye-hand coordination
- Improve overall endurance and muscle strengthening
- Substitution and coping skills

Vestibular Therapy can Treat:
- Benign Paroxysmal Positional Vertigo (BPPV)
- Post-Concussion Syndrome
- Abnormal Gait
- Multiple Sclerosis
- Acoustic Neuroma
- Parkinson’s Disease
- Labyrinthitis
- Vestibular Neuritis
- Migraine Related Motion Sickness
- Vestibular Weakness
- Mild Traumatic Brain Injury
WinBack Therapy
What is WinBack Tecartherapy?
WinBack Tecartherapy is a cutting-edge modality that harnesses high-frequency, non-invasive energy to stimulate the body’s natural healing processes using electrical currents. This form of therapy is particularly effective in alleviating pain associated with inflammation. By triggering a nerve signal through deep heat, WinBack Therapy activates the body’s natural cellular ability to repair itself, providing a warm and soothing sensation throughout the body and relief in the brain. What sets WinBack apart is its versatility, enabling therapists to integrate hands-on treatment during therapy.
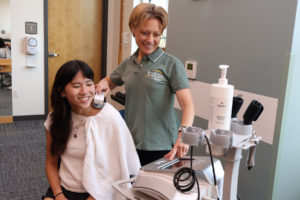
Benefits of WinBack Therapy:
- Reduces pain
- Reduces inflammation
- Restores movement
- Increases blood flow
Work Related Rehabilitation
Physical Therapy at St. Luke’s offers a wide variety of services for employees and employers to improve the rehabilitation process from prevention services to post injury recuperation.
As an employer, if you need pre–employment screening, on–site job analysis, or prevention programs, we are the right partner for you. We are committed to keeping the communication and scheduling process as smooth as possible with all members of the Occupational Rehabilitation team including the patient, the physician, the claims manager, the vocational service provider, and/or the insurer.
We perform a Functional Capacity Evaluation (FCE) to rapidly determine if a patient can work, and if so, at what physical level. FCE’s can be completed for any of the following reasons:
- Before rehabilitation to determine rehab needs
- After rehabilitation to determine a safe return to work
- To complete a disability determination and define an individual’s employability
- Independent medical evaluations
Schedule an Appointment
Our experienced team at Physical Therapy at St. Luke's is here to help you on your journey to recovery and improved mobility.
Schedule